RCM Healthcare: Complete Guide to Revenue Cycle Management
Last Updated on: February 23, 2026
Reviewed by Kyle Wilson
- Licensed Agent
- @ verimedix

RCM healthcare refers to the financial process that healthcare providers use to manage patient billing, claims, and payments from start to finish. It helps hospitals, clinics, and medical practices improve revenue, reduce errors, and maintain financial stability. Today, healthcare RCM is essential for ensuring accurate reimbursements and smooth administrative operations.
With growing complexities in insurance policies and compliance rules, healthcare organizations are increasingly adopting advanced revenue cycle strategies. By implementing efficient RCM systems, providers can reduce claim denials, improve cash flow, and focus more on delivering quality patient care.
Get Free Quotes
Customized Options Await
What is RCM in Healthcare?
Revenue cycle management (RCM) in healthcare is the process of tracking patient revenue from appointment scheduling to final payment. It includes insurance verification, coding, claim submission, and payment collection.
An effective RCM system ensures that healthcare providers receive accurate and timely reimbursements. It also improves patient satisfaction by offering clear billing and transparent communication.
RCM Meaning in Healthcare
RCM stands for revenue cycle management, which focuses on managing the financial side of healthcare services. It covers all stages of patient billing and insurance claim processing. A strong understanding of RCM healthcare means it helps providers optimize financial performance and reduce administrative challenges.
Full Form of RCM in Medical Terms
The full form of RCM in medical terms is revenue cycle management. This process involves multiple steps such as patient registration, eligibility checks, coding, billing, and payment posting. Each step plays a critical role in maintaining financial health in medical organizations.
Importance of RCM in Modern Healthcare
In modern healthcare, RCM ensures accurate billing and compliance with insurance regulations. It helps reduce claim denials and improves operational efficiency. By implementing proper RCM strategies, providers can focus more on patient care and less on administrative burdens.
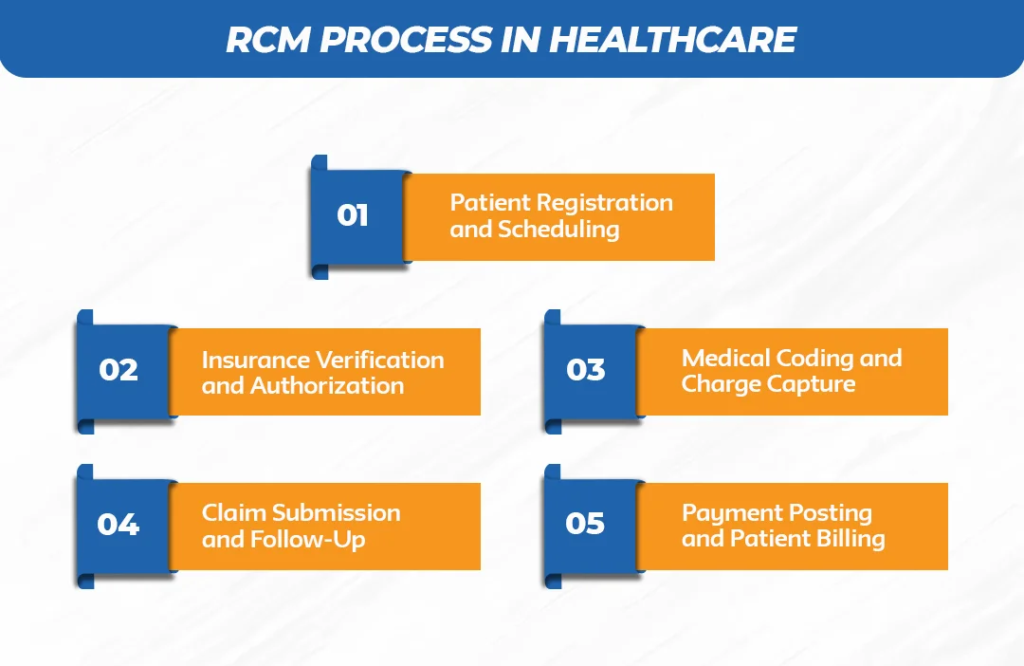
RCM Process in Healthcare
The RCM process in healthcare includes several steps that ensure providers receive payment for services delivered. Each stage must be handled carefully to avoid errors and delays.
Patient Registration and Scheduling
The process begins when a patient schedules an appointment. Accurate data collection during registration reduces billing mistakes and claim rejections. It also ensures proper documentation and smoother claim processing later.
Insurance Verification and Authorization
Insurance verification confirms patient eligibility and coverage details. This step prevents claim denials and ensures that providers receive payments without delays. Prior authorization is also necessary for certain treatments.
Medical Coding and Charge Capture
Medical coding converts patient diagnoses and procedures into standardized codes. Accurate coding ensures compliance and correct reimbursement. It also helps healthcare organizations avoid audits and penalties.
Claim Submission and Follow-Up
After coding, claims are submitted to insurance companies. Continuous follow-up ensures faster payment and reduces denials. Effective claim management improves cash flow and financial performance.
Payment Posting and Patient Billing
Payments are recorded, and patients are billed for any remaining balance. Transparent billing improves patient satisfaction and trust. It also helps healthcare providers maintain consistent revenue.
Healthcare RCM Services
Healthcare RCM services include a range of solutions designed to improve billing accuracy and efficiency. These services help providers focus on patient care while experts manage financial operations.
End-to-End Revenue Cycle Solutions
Many RCM healthcare services cover the entire revenue cycle. This includes registration, coding, billing, denial management, and reporting. Comprehensive solutions improve efficiency and reduce administrative workload.
Denial Management and Appeals
Denial management identifies and resolves claim issues. Experts analyze root causes and implement corrective strategies. This helps healthcare organizations recover lost revenue and improve claim success rates.
Compliance and Regulatory Support
RCM providers ensure compliance with healthcare regulations. They stay updated with coding changes, insurance policies, and industry standards. This reduces legal risks and protects financial stability.
Analytics and Performance Reporting
Advanced reporting tools provide insights into financial performance. Providers can track key metrics, identify gaps, and optimize revenue cycle strategies. Data-driven decisions lead to long-term growth.

Benefits of Healthcare RCM
Healthcare RCM offers numerous advantages for providers and patients. It improves operational efficiency and financial performance.
Improved Revenue and Cash Flow
Effective revenue cycle management ensures faster reimbursements and reduced revenue leakage. Providers can maintain stable financial operations and growth.
Reduced Claim Denials
Accurate documentation and coding reduce claim rejection rates. This increases approval rates and minimizes financial losses.
Enhanced Patient Experience
Transparent billing and communication improve patient trust and satisfaction. Patients feel more confident when they understand their financial responsibilities.
Better Compliance and Risk Management
RCM systems ensure compliance with healthcare regulations. This reduces audit risks and protects healthcare organizations from penalties.
Healthcare RCM Software and Technology
Technology plays a vital role in modern healthcare RCM solutions. Automation and artificial intelligence improve efficiency and accuracy.
Cloud-Based RCM Systems
Cloud technology allows secure access to patient and billing data. It enhances collaboration and reduces infrastructure costs. Healthcare providers can manage operations remotely and efficiently.
AI and Automation in RCM
Automation reduces manual errors and speeds up billing processes. AI tools can predict denials and improve claim accuracy. This leads to better financial outcomes.
Integration with EHR Systems
Integration with electronic health records improves data accuracy. It ensures seamless communication between clinical and financial departments. This enhances workflow and operational efficiency.
RCM Outsourcing for Healthcare Providers
Many healthcare organizations choose to outsource RCM services to specialized companies. This approach reduces administrative workload and improves financial performance.
Cost-Effective Revenue Cycle Solutions
Outsourcing reduces staffing and training costs. It also improves operational efficiency and profitability. Healthcare providers can allocate resources to patient care.
Access to Skilled Professionals
RCM outsourcing provides access to experienced billing and coding experts. These professionals stay updated with industry trends and regulations. This ensures accurate and compliant billing.
Scalability and Flexibility
Outsourcing allows providers to scale services based on their needs. It supports business growth and adapts to changing healthcare demands.
Focus on Core Healthcare Services
By outsourcing RCM, providers can focus on delivering quality care. Administrative burdens are handled by experts, improving overall productivity.
Conclusion
RCM healthcare is essential for improving financial performance, reducing claim denials, and ensuring compliance in today’s complex medical environment. A well-structured revenue cycle helps healthcare providers streamline operations and enhance patient satisfaction.
By implementing advanced RCM solutions and outsourcing when needed, healthcare organizations can achieve long-term growth and stability. Investing in efficient revenue cycle management is a strategic step toward better healthcare and stronger financial outcomes.Contact Verimedix today to streamline your healthcare RCM and achieve faster, more reliable revenue growth.
FAQs
What is RCM in healthcare?
RCM in healthcare refers to revenue cycle management, which is the process of handling all financial activities related to patient care. It starts from patient registration and insurance verification and continues through medical coding, claim submission, payment posting, and patient billing.
What does RCM stand for in medical terms?
In medical terms, RCM stands for revenue cycle management. It focuses on managing the financial lifecycle of healthcare services, ensuring that providers receive accurate and timely payments for the care they deliver.
What services does RCM healthcare provide?
Healthcare RCM services include patient registration, insurance eligibility verification, medical coding, charge capture, claim submission, denial management, payment posting, and patient billing. These services help healthcare providers streamline financial processes, improve accuracy, and increase overall revenue.
What is the full meaning of RCM?
The full meaning of RCM is revenue cycle management. It represents the complete financial process in healthcare, covering every stage from patient scheduling to final payment. A well-managed revenue cycle ensures accurate billing, faster reimbursements, better compliance, and improved patient satisfaction.
THE AUTHOR
Shawn Davis is a leading expert in medical administration and revenue optimization. For years, Shown has been driving outstanding financial outcomes for healthcare providers through Denial Management, Eligibility Verification, Medical Billing and Coding, and Revenue Cycle Management. He is dedicated to helping practices streamline their operations and maximize their reimbursements through precision-driven digital solutions.



